also information, submitting files, checking out information, and also exchanging messages with other individuals. 문자사이트
Dentists
Your dentist can help you decide when you’ll need treatment, and r 교정전문치과 whether you have options that are less invasive or more discreet.
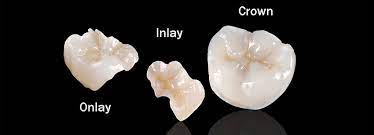
Porcelain Inlays
they are used to correct cracked or damaged teeth. 교정전문치과 dental office.
Basic of Massage Therapy Treatment
Massage therapy must ideally be complied with through a bathroom along with warm water. 부천 스웨디시
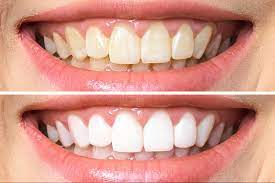
Teeth Whitening
The biggest disadvantage is that the level of whitening is restricted by the amount of gel provided. Also, the gel provided is very abrasive 교정 전문 치과(even bleach), and could in some cases, weaken tooth enamel.
Methods for Keeping Track of Your Associate Recommendations
Even if you remain in associate advertising and marketing doesn’t indicate all your associate recommendation prospecting techniques are limited online. Offline tasks can be exceptionally helpful for generating leads. 비트겟 사용법
먹튀검증사이트 Online Sports Betting Line Service
This uses the wagerers the possibility to keep track of the video games or events she or he intends to bet on. 먹튀검증사이트
Aromatherapy Massage Therapy New York City
Aromatherapy Massage New York City: Back to Fundamentals Massage massagesiheung.com
태국여행 Path 62– Through Car
If you possess the methods and desire to perform the trip adequately, look at tapping the services of a 4×4. You can make use of the country’s a lot of off-road keep tracks of along the road for incorporated experience, and the contemporary 4x4s are roomy, cool as well as deal convenience plus toughness– the best combination for your trip vacation. www.태국여행.com
zerobacktv Bird Seeing in Arizona
The spot is additionally best if you intend to find unusual kinds of birds including periodic varieties of kingbirds, chickadees, becards, gnatcatchers, titmice, sparrows, tanagers, as well as warblers. zerobacktv
Acquire A Massage Therapy In Sedona
Centered Tissue Massage – massage therapy of the much deeper musculature and also combinative cells to launch persistent strain as well as ache. It is usually a stronger massage therapy that is enjoyed by knowledgeable customers. Prenatal/Pregnancy Massage Massage therapy for the mother-to-be assists her to lessen aches and also soreness throughout the maternity. Neuromuscular […]
Receive A Massage Therapy In Bradenton
Bradenton, Florida, merely southern of Tampa Bay on Florida’s west shore, is a wonderful location to obtain great massage treatment. Massage therapy in Bradenton is commonly readily available coming from private State Licensed Massage Therapists, Licensed Massage Establishments, and also numerous realm course Day Spas. Whether your target is actually to entirely kick back along […]
Obtain A Massage Therapy In Boston ma
Obtaining a massage therapy in Boston is a momentous and also fully pleasurable take that is one thing you will certainly prefer to replay over as well as over since it experiences excellent as well as possesses remarkable health and wellness advantages. Whether your target is actually to fully unwind along with sluggish, comforting massage […]
Acquire A Massage Therapy In Longmont
Whether you go to Longmont for service travel, a remarkable holiday, or even a household move you may locate you yearn to acquire massage treatment. Massage therapy in Longmont is extensively offered to come from individual Certified Massage Therapists, Massage Establishments, and also an increasing variety of Day Spas. Swedish Massage Resting massage therapy utilizes […]
Acquire A Massage Therapy In Upland
Certainly not merely may you get a Deep Tissue massage therapy you can easily likewise obtain Shiatsu and also various other types of massage therapy in this attractive southerly California area. Massage therapy in Upland is extensively on-call coming from private Licensed as well as Certified Massage Therapists, Massage Establishments, as well as a variety […]